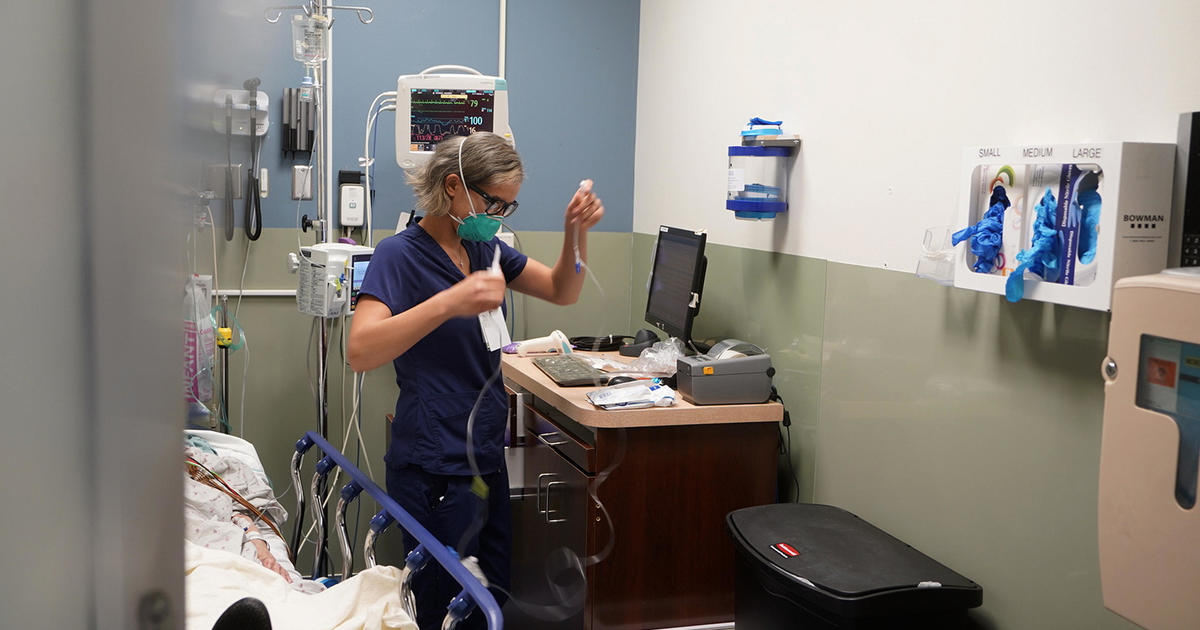
Trump Administration Allows States To Make Medicaid Recipients Work
(CNN Money) -- The Trump administration will allow states for the first time to impose work requirements on Medicaid recipients.
The Centers for Medicare & Medicaid Services released a guidance Thursday outlining what states need to do to mandate that certain Medicaid enrollees work to qualify for benefits. The agency is expected to start approving state waivers promoting "community engagement activities" in coming weeks.
The historic move would be a significant change in how the government health insurance program operates and would fulfill a longtime Republican goal. States, for instance, could require non-disabled, working age recipients to work, volunteer, go to school or enter a job training program. The guidance also includes caregiving as one of the activities.
"Medicaid needs to be more flexible so that states can best address the needs of this population. Our fundamental goal is to make a positive and lasting difference in the health and wellness of our beneficiaries, and today's announcement is a step in that direction," said Seema Verma, the agency's administrator.
Critics, however, argue that Republicans are using work requirements to thin the Medicaid rolls. They fear many recipients will be unable to meet the mandate and be left uninsured. The work requirements will likely be challenged in court.
In its guidance, CMS pointed to studies that show working and volunteering can contribute to better health as justification that the requirement is in keeping with Medicaid's mission.
The agency's guidance provides states with a lot of flexibility in designing their programs and highlights that many recipients may need additional considerations.
For instance, the guidance notes that some Medicaid recipients may have trouble meeting these requirements because of poor health, substance abuse or high unemployment in their areas. States should take these issues -- as well as recipients' employability -- into consideration and allow for modifications or exemptions, the agency said. Pregnant women will also be exempt.
The agency specifically calls out the opioid epidemic, saying that time spent in treatment can count towards the mandate and those in intensive recovery programs can be excused. Many governors, including Republican ones, have defended the Medicaid program as being critical to addressing the substance abuse crisis.
States will be required to describe strategies to assist recipients in meeting the requirements and to link them to job training and support resources, including child care and transportation. However, they will not be allowed to use federal Medicaid funding to finance these services.
The agency is encouraging states to align their Medicaid work requirements with those mandated by other federal safety net programs. Recipients who meet the work requirements in the Supplemental Nutrition Assistance Program, commonly known as food stamps, and by the Temporary Assistance for Needy Families, must be considered in compliance with their state's Medicaid rules.
Republicans have long wanted to add work requirements to the Medicaid program, which covers nearly 75 million low-income children, adults, elderly and disabled Americans. The broadening of Medicaid to low-income adults under Obamacare -- roughly 11 million have gained coverage under the health reform law's Medicaid expansion provision -- further spurred GOP efforts.
However, the Obama administration did not approve any state waivers that would impose work mandates, saying it was not in keeping with the program's mission to provide access to medical services. Consumer advocates and health policy experts fear that such a requirement could prove a big hurdle for many recipients, leaving them without the care they need.
The Trump administration swiftly signaled that it held a different view. Verma, sent a letter to governors hours after after she was confirmed in March urging them to apply for such waivers.
Related: Trump administration open to making some Medicaid recipients work, pay premiums
"One of the things that states have told us time and time again is that they want more flexibility to engage their working-age, able-bodied citizens on Medicaid," Verma told a conference of state Medicaid directors in November. "They want to develop programs that will help them break the chains of poverty and live up to their fullest potential. We support this."
The guidance release Thursday pointed to several studies that said unemployment is harmful to one's health and can prompt higher rates of hospital admission and death, as well as poorer general and mental health.
Ten states -- Arizona, Arkansas, Indiana, Kansas, Kentucky, Maine, New Hampshire, North Carolina, Utah and Wisconsin -- have submitted waivers that include work or community engagement requirements, according to the agency. South Dakota's governor said in his State of the State address Tuesday that he would also look to require certain recipients to work.
Verma, who served as a Medicaid consultant for Indiana and Kentucky before joining the Trump administration, has long advocated for work requirements. Now, she is in a position to approve them.
"For the future of our country, we need all Americans to be active participants in their communities," she said in November. "Believing that community engagement requirements do not support or promote the objectives of Medicaid is a tragic example of the soft bigotry of low expectations consistently espoused by the prior administration. Those days are over."
Related: Millions of Medicaid recipients already work
Many Medicaid recipients are already employed. Some 60% of non-disabled, working-age adults have jobs, while nearly 80% live in families with at least one member in the labor force, according to a Kaiser Family Foundation analysis. Most of those who don't work cite illness, disability or family obligations as the reason.
The work requirements will likely have an impact on a broad number of adults. Many Medicaid enrollees may have physical or mental health problems -- such as arthritis or asthma -- that don't meet the criteria for federal disability programs, but still interfere with their ability to work, Kaiser said. They could find it difficult to apply for exempt status and verify it, which may need to be done monthly in some states, while those who are working may have a hard time verifying their hours, especially if they have variable shifts.
Plus, state Medicaid agencies won't get any additional federal funding to help recipients find and hold jobs, even though they are generally not equipped to develop, provide, and administer work support programs, said MaryBeth Musumeci, associate director of Kaiser's Program on Medicaid and the Uninsured.
"The new [state programs] will penalize individuals by having them lose health coverage, rather than incentivize them, as a voluntary program with adequately funded supportive services necessary to overcome barriers, would," she said.
The-CNN-Wire
™ & © 2018 Cable News Network, Inc., a Time Warner Company. All rights reserved.